External Quality Review (EQRO)
For more than 50 years, Qsource has been working with state Medicaid agencies to enhance the value of healthcare services provided to the Medicaid managed care population.
Qsource is a designated, independent External Quality Review Organization (EQRO) helping state agencies meet federal regulations for assessing managed care organizations (MCOs), prepaid inpatient health plans (PIHPs), and prepaid ambulatory health plans (PAHPs).
Qsource evaluates and aggregates information on the timeliness, access, and quality of healthcare services furnished to Medicaid enrollees as required by the code of federal regulations 42 CFR Part 438, Subpart E and Centers for Medicare & Medicaid (CMS).
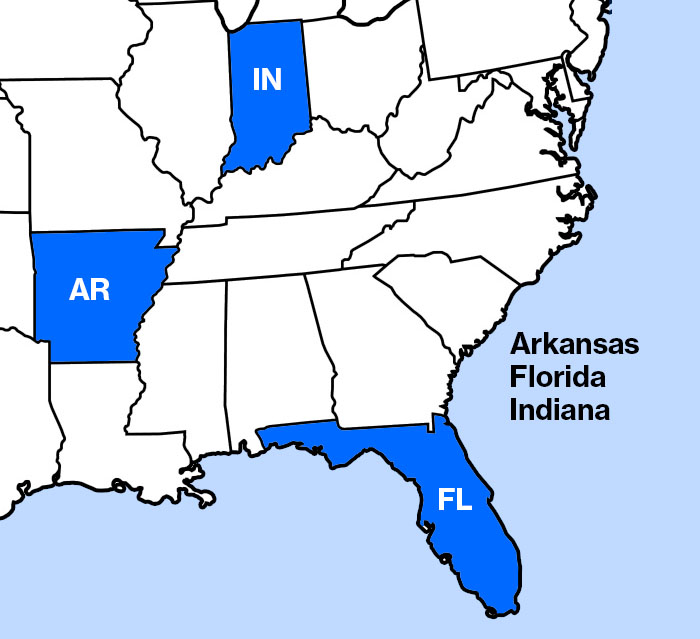
Qsource is the EQRO in three states, Arkansas, Indiana, and Florida- Florida Healthy Kids Corp. With our national subject matter experts, data analysts and proven processes, we know how to partner with you to improve performance.
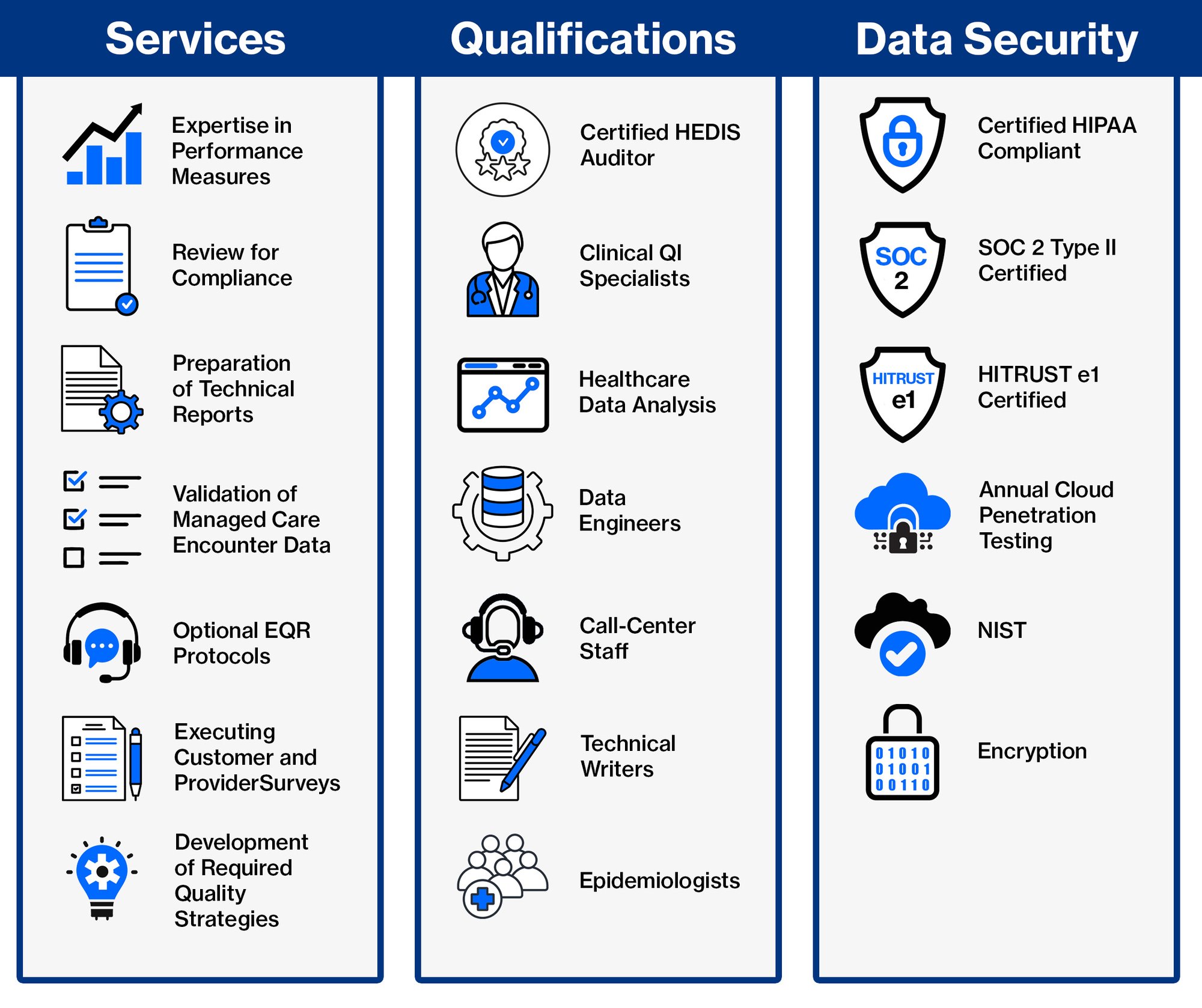
The EQR process currently consists of four mandatory activities and six optional activities, in addition to producing an annual EQR technical report and providing technical assistance, as needed. Each of the mandatory and optional activities has a corresponding CMS EQR protocol, which Qsource follows when performing each EQR activity.
We have helped several states establish their EQR programs and have worked with them throughout their transitions to new managed care models by conducting readiness reviews and providing technical assistance and program guidance.
As an External Quality Review Organization and a QIO-like organization, we have worked with states and MCOs in virtually every area of operations and management. We use data analysis, audits and technical assistance to improve MCO and network performance.